Bunnie Xo Facelift Plastic Surgery Stunned Husband Jelly Roll

The Bunnie Xo facelift story stands out because it is built on confirmed details, not assumptions. Bunnie Xo, known for her Dumb Blonde podcast and her connection to Jelly Roll, openly shared that she underwent a facelift in 2026 and documented the process herself. That level of transparency gives a clearer understanding of what the procedure and recovery actually involve, especially in a space where information is often filtered or incomplete.
What makes the Dumb Blonde podcast host’s experience different is the way she combined personal storytelling with real-time updates. Instead of presenting only final results, she showed the full facelift process, including the decision-making stage, the role of previous filler, and the reality of post-operative healing.
Key Takeaways of Bunnie Xo Facelift Plastic Surgery
- Bunnie Xo, Jelly Roll’s wife, publicly confirmed undergoing a facelift, providing rare firsthand details about her recovery process including swelling and bruising.
- Her decision stemmed from dissatisfaction with old filler treatments, highlighting the limits of non-surgical fixes over time.
- Bunnie’s candid updates offer a realistic view of facelift recovery, dispelling misconceptions that cosmetic surgery results are immediate or flawless.
- Her openness about surgery alongside her advocacy for self-love presents a balanced perspective on choosing cosmetic procedures.
- Bunnie Xo’s marriage to Jelly Roll increased public attention, turning a personal medical choice into a widely discussed celebrity topic.
Who Is Bunnie Xo (real name Alisa DeFord)?
Bunnie Xo (real name Alisa DeFord), born January 22, 1980, is an American podcast host and media producer best known for the Dumb Blonde Podcast. She is the founder of Dumb Blonde Productions, where she leads an interview-based platform centered on long-form conversations with guests from the music and entertainment industries.
Through her direct and unfiltered style, she has built a strong following across social media and podcast platforms. In addition to podcasting, she has expanded her presence as a content creator and entrepreneur, growing her media brand into a recognized name within digital entertainment.
“Jelly Roll’s Wife” Bunnie Xo
Bunnie Xo is also widely recognized as the wife of country singer Jelly Roll (Jason DeFord), whom she married in 2016. Her public profile grew alongside his rising music career, but she has established her own audience independently through social media, YouTube, and podcasting.
She has been open about her personal journey, including past struggles, career changes, and her transition into a successful media business, topics she also explores in her 2026 memoir Stripped Down: Unfiltered and Unapologetic.
Bunnie XO Shares SHOCKING Plastic Surgery Results. Video Source: Entertainment Tonight (ET).
Bunnie Xo Shares Face Lift Journey
Bunnie Xo began talking about her facelift before the procedure ever happened, giving her audience early insight into her decision. In a March 13, 2026 episode of her Dumb Blonde podcast, she openly confirmed that she had a facelift scheduled for March 15 and asked listeners for support ahead of surgery. She stated, “I’m asking for lots of prayers… I’m having a facelift,” making it clear this was a planned step rather than a last-minute decision.
Issues with Her Old Fillers
She also explained that the idea had been on her mind for years, largely due to ongoing issues with previous filler treatments. In her own words, she shared that dissolving filler over time had only “improved slightly,” which led her to move away from temporary fixes and toward a more definitive option. That context matters because it shows the facelift was not impulsive, but part of a longer process of trying to correct and reset her facial appearance.
After the procedure, Bunnie Xo continued documenting the journey in real time. She posted updates showing swelling, bruising, and bandaging, while also describing how recovery felt physically. In one update, she said she felt extremely tight, even describing the sensation as being “choked,” and shared that she was sleeping in a recliner during early healing. That level of detail gave her audience a clear, firsthand look at what recovery actually involves, from the initial discomfort to the gradual improvement over time.
Bunnie Xo’s Appearance After Facelift Procedure
Public conversation around Bunnie Xo’s appearance grew after she shared both polished content and unfiltered recovery updates following her procedure. The contrast between her usual camera-ready look and early healing stages gave viewers a clearer view of what post-surgical recovery can actually look like.
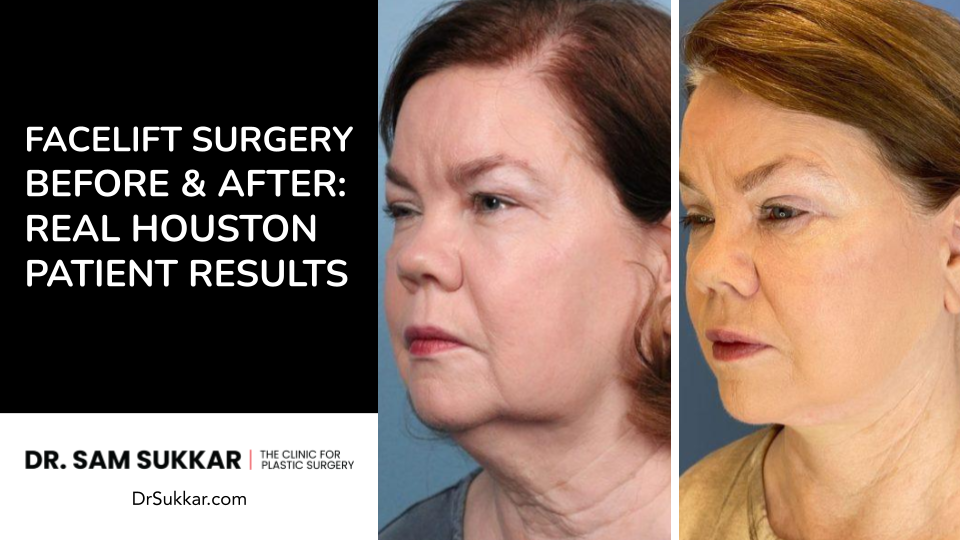
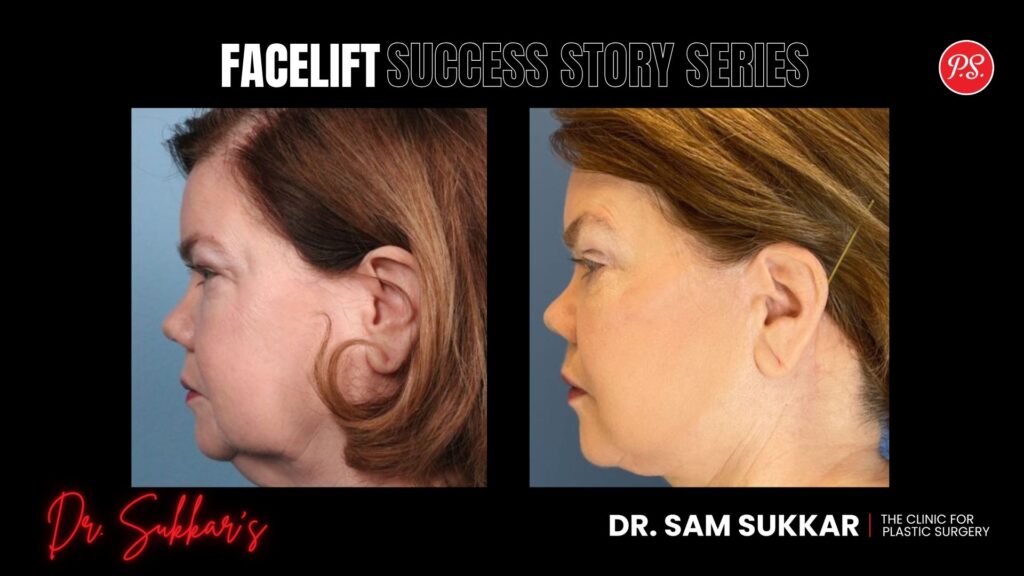
Facelift Bunnie Xo Photos and Visible Post-Op Changes
Bunnie Xo’s appearance after her facelift drew attention because she chose to show the reality of recovery instead of hiding it behind polished content. After confirming the procedure, she posted updates that showed visible swelling, bruising, bandaging, and tightness across the lower face and neck, giving followers a rare look at what the early healing phase can actually involve.
Her openness made the changes easier to understand in context: this was not a final result, but a normal post-surgical stage immediately after a major facial procedure.
Why Her Facelift Went Viral
When Bunnie Xo reveals her facelift plans in a March 13 episode of her podcast, social media followers immediately took notice. Her willingness to document everything, from surgical pen markings to drainage tubes, made the story impossible to ignore.
Why it captured attention:
- She’s always said “yes i love natural bodies” while being transparent about implants, a BBL, and fillers
- The raw footage contrasted sharply with typical polished cosmetic content
Jelly Roll’s Wife Bunnie Xo Shares Raw Look at Facelift Recovery. Video Source: E! News.
What made her coverage stand out was how directly she described the experience. In follow-up recovery updates, she said facial tightness made her feel like she was being “choked,” and reports noted that she discussed sleeping in a recliner and dealing with the physical strain that can come with early healing. That kind of documentation gave the public a more accurate picture of facelift recovery, showing that the swollen, bruised stage comes before the refined result people usually see later.
What Bunnie Xo Has Publicly Shared About Cosmetic Work
Unlike many celebrity stories about plastic surgery, this one includes direct comments from Bunnie and from her surgeon.
What Bunnie Xo reveals about her facelift procedure
In an episode of her podcast and on social media, Bunnie XO reveals that old filler was one of the main reasons she decided to get a facelift. She said that for the past three years, filler had been dissolved multiple times but only improve slightly.
Bunnie explained that she did not want to keep layering fixes on top of past cosmetic procedures. She has also spoken about self love and saying “yes, I love natural bodies,” while still being open about choosing surgery for herself.
Recovery details Bunnie shared after surgery
Bunnie Xo shared detailed updates during her recovery, giving a clear picture of what the early post-operative phase involved. Her updates were unusually candid. She also compared herself to Bert Kreischer, and described feeling a tight or choking sensation from ear to ear during post op recovery. She also said she was bruised, extremely swollen, and dealing with breathing issues and cabin fever.
Bunnie Xo’s Husband Jelly Roll (real name Jason Bradley DeFord) and His Weight Loss Transformation
Bunnie Xo’s husband, country singer Jelly Roll (real name Jason Bradley DeFord), has gained attention for his weight loss transformation. As his career continued to grow, he placed more focus on improving his health through changes in diet and lifestyle. Fans have noticed a leaner appearance along with increased energy during performances and public appearances.
During an episode of the Dumb Blonde podcast, he and Bunnie Xo spoke openly about his weight and overall health. He set a personal goal for himself and discussed the importance of staying accountable, while Bunnie supported the conversation with honesty and encouragement. Their dynamic made the topic feel real and relatable. This shows how open communication and shared support can play a role in long-term lifestyle changes.
As of early 2026, singer Jelly Roll has made a dramatic transformation, reportedly losing around 275 pounds. He went from over 540 pounds to approximately 265 pounds. His progress has come from consistent daily effort. He mentioned that he walks and runs about 2-3 miles a day, along with major changes to his diet. He has focused on higher-protein meals, reduced alcohol intake, and committed to building sustainable habits.
Jelly Roll’s 275lb Transformation – A Year For a Life. Video Source: Men’s Health.
Frequently Asked Questions About Bunnie Xo Facelift Plastic Surgery Stunned Husband Jelly Roll
What cosmetic procedure did Bunnie Xo undergo in 2026?
Bunnie Xo underwent a facelift procedure. The procedure addressed areas like her mid face, cheeks, neck, jawline, temples, and upper eyelids to achieve a refreshed look.
Why did Bunnie Xo decide to get a facelift instead of continuing with fillers?
She chose a facelift after years of dissolving old filler that only improved her appearance slightly. Also, she didn’t want to keep layering temporary fixes on top of previous cosmetic work.
How long will a facelift last?
Facelift can last around 10-to-15 years in many patients, depending on skin, lifestyle, and how well deeper tissues were repositioned. The procedure resets facial aging, but natural aging continues over time.
How painful is a face lift?
A facelift is generally not described as highly painful. Most patients report tightness, soreness, and mild to moderate discomfort during the first few days. These symptoms are usually managed with prescribed medication.
Conclusion and Summary of Bunnie Xo Facelift Plastic Surgery Stunned Husband Jelly Roll
The Bunnie Xo’s facelift story is important because it is grounded in what she personally shared, not outside interpretation. From discussing filler concerns to documenting recovery, she provided clear insight into why she chose surgery. Also, Bunnie showed how the process really looked like step by step. That level of openness helps set realistic expectations about swelling, healing, and the time it takes to see final results.
Her experience also shows how a facelift can be part of a broader, thoughtful approach to appearance. Rather than relying on repeated temporary fixes, she chose a more comprehensive solution aligned with her goals. Clear information, realistic expectations, and a well-planned approach make a meaningful difference in how results are achieved.
Your Trusted Destination for Facelift Surgery in Houston, Texas (TX)
Are you located in one of these Houston Metro Area cities?
Houston, The Woodlands, Sugar Land, Katy, Pearland, Pasadena, League City, Baytown, Conroe, Cypress, Spring, Kingwood, Humble, Missouri City, Friendswood, Bellaire, Clear Lake, Tomball, Galveston, Richmond, Rosenberg, Stafford, La Porte, Deer Park, Seabrook, Webster, Alvin, and Channelview.
Board-Certified Plastic Surgeon Dr. Sam Sukkar, MD, FACS, and the The Clinic for Plastic Surgery Team provide advanced facelift surgery solutions to rejuvenate and restore a more youthful, refreshed appearance.
If you are dealing with sagging skin, deep facial folds, jowls, volume loss, or a tired, aging appearance, we offer comprehensive facial rejuvenation options, including:
- Facelift Surgery
- Mini Facelift
- Lower Facelift
- Neck Lift Surgery
- Facelift with Neck Lift
- Customized Facial Rejuvenation Treatment Plans
Visit our modern 18,000+ sq. ft. plastic surgery center and med spa in Houston, Texas, designed for comfort, privacy, and results-driven care. From your first consultation through recovery, our talented team focuses on natural-looking rejuvenation with elegant, refreshed results.
For patients outside the Houston area or those with limited availability, schedule a virtual facelift surgery consultation.
Book Your Personalized Facelift Consultation today at DrSukkar.com or call (281) 940-1535.
About the Author – Meet Dr. Sam Sukkar, MD

Dr. Sam Sukkar, MD, FACS is a highly respected Board-Certified Plastic Surgeon in Houston, Texas, known for his expertise in advanced cosmetic and reconstructive procedures. As the founder of The Clinic for Plastic Surgery, Dr. Sukkar has set a new standard for excellence, performing over 20,000 procedures with a focus on delivering natural, refined results.
Dr. Sukkar earned his Doctor of Medicine (M.D.) degree from Louisiana State University School of Medicine in 1992 after graduating summa cum laude with a Bachelor of Science in Microbiology. He then completed an intensive General Surgery Residency at the University of Texas Hermann Hospital before being selected for a highly competitive Plastic Surgery Fellowship at Northwestern University in Chicago, one of the most prestigious training programs in the country.
With more than 20 years of experience, Dr. Sukkar is a Diplomate of the American Board of Plastic Surgery and a Fellow of the American College of Surgeons (FACS). He is also an active member of the American Society of Plastic Surgeons (ASPS) and the Houston Society of Plastic Surgery (HSPS). His dedication to innovation and continuing education has solidified his reputation as a leading expert in aesthetic surgery, specializing in breast surgery, body contouring, facial procedures, and non-invasive treatments.
Dr. Sukkar’s expertise has been recognized by Houston Magazine, naming him one of Houston’s “Top Docs for Women,” and he has been featured among RealSelf’s America’s Top Doctors. Committed to his patients, he prioritizes personalized care, ensuring every individual feels informed, comfortable, and confident in their aesthetic journey.
Contact Dr. Sukkar today to schedule a consultation, visit DrSukkar.com to learn more, or call us directly at (281) 940-1535.
Cover Image Illustration (Conceptual Representation) by: Dr. Sam Sukkar, MD, The Clinic for Plastic Surgery.